Smartphone-powered microchip for at-home medical diagnostic testing developed
The new technology could make at-home diagnosis of diseases faster and more affordable: Researchers working with startup GRIP Molecular Technologies
Advertisement
A University of Minnesota Twin Cities research team has developed a new microfluidic chip for diagnosing diseases that uses a minimal number of components and can be powered wirelessly by a smartphone. The innovation opens the door for faster and more affordable at-home medical testing.

A University of Minnesota Twin Cities research team has developed a new microfluidic chip for diagnosing diseases that uses a minimal number of components and can be powered wirelessly by a smartphone. The innovation opens the door for faster and more affordable at-home medical testing (symbolic image).
Unsplash

A University of Minnesota Twin Cities research team has developed a new microfluidic chip for diagnosing diseases that uses a minimal number of components and can be powered wirelessly by a smartphone.
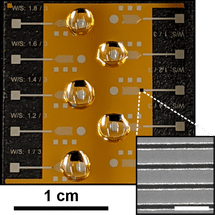
Laboratory of Nanostructures and Biosensing, University of Minnesota

The researchers’ paper is published in Nature Communications. Researchers are also working to commercialize the technology.
Microfluidics involves the study and manipulation of liquids at a very small scale. One of the most popular applications in the field is developing “lab-on-a-chip” technology, or the ability to create devices that can diagnose diseases from a very small biological sample, blood or urine, for example.
Scientists already have portable devices for diagnosing some conditions—rapid COVID-19 antigen tests, for one. However, a big roadblock to engineering more sophisticated diagnostic chips that could, for example, identify the specific strain of COVID-19 or measure biomarkers like glucose or cholesterol, is the fact that they need so many moving parts.
Chips like these would require materials to seal the liquid inside, pumps and tubing to manipulate the liquid, and wires to activate those pumps—all materials that are difficult to scale down to the micro level. Researchers at the University of Minnesota Twin Cities were able to create a microfluidic device that functions without all of those bulky components.
“Researchers have been extremely successful when it comes to electronic device scaling, but the ability to handle liquid samples has not kept up,” said Sang-Hyun Oh, a professor in the University of Minnesota Twin Cities Department of Electrical and Computer Engineering and senior author of the study. “It’s not an exaggeration that a state-of-the-art, microfluidic lab-on-a-chip system is very labor intensive to put together. Our thought was, can we just get rid of the cover material, wires, and pumps altogether and make it simple?”
Many lab-on-a-chip technologies work by moving liquid droplets across a microchip to detect the virus pathogens or bacteria inside the sample. The University of Minnesota researchers’ solution was inspired by a peculiar real-world phenomenon with which wine drinkers will be familiar—the “legs,” or long droplets that form inside a wine bottle due to surface tension caused by the evaporation of alcohol.
Using a technique pioneered by Oh’s lab in the early 2010s, the researchers placed tiny electrodes very close together on a 2 cm by 2 cm chip, which generate strong electric fields that pull droplets across the chip and create a similar “leg” of liquid to detect the molecules within.
Because the electrodes are placed so closely together (with only 10 nanometers of space between), the resulting electric field is so strong that the chip only needs less than a volt of electricity to function. This incredibly low voltage required allowed the researchers to activate the diagnostic chip using near-field communication signals from a smartphone, the same technology used for contactless payment in stores.
This is the first time researchers have been able to use a smartphone to wirelessly activate narrow channels without microfluidic structures, paving the way for cheaper, more accessible at-home diagnostic devices.
“This is a very exciting, new concept,” said Christopher Ertsgaard, lead author of the study and a recent CSE alumnus (ECE Ph.D. ‘20). “During this pandemic, I think everyone has realized the importance of at-home, rapid, point-of-care diagnostics. And there are technologies available, but we need faster and more sensitive techniques. With scaling and high-density manufacturing, we can bring these sophisticated technologies to at-home diagnostics at a more affordable cost.”
Oh’s lab is working with Minnesota startup company GRIP Molecular Technologies, which manufactures at-home diagnostic devices, to commercialize the microchip platform. The chip is designed to have broad applications for detecting viruses, pathogens, bacteria, and other biomarkers in liquid samples.
“To be commercially successful, in-home diagnostics must be low-cost and easy-to-use,” said Bruce Batten, founder and president of GRIP Molecular Technologies. “Low voltage fluid movement, such as what Professor Oh’s team has achieved, enables us to meet both of those requirements. GRIP has had the good fortune to collaborate with the University of Minnesota on the development of our technology platform. Linking basic and translational research is crucial to developing a pipeline of innovative, transformational products.”
Original publication
Other news from the department science
Most read news
More news from our other portals
Something is happening in the life science industry ...
This is what true pioneering spirit looks like: Plenty of innovative start-ups are bringing fresh ideas, lifeblood and entrepreneurial spirit to change tomorrow's world for the better. Immerse yourself in the world of these young companies and take the opportunity to get in touch with the founders.





























































