BAFfling cancer growth strategies: new targets for chromatin remodeling mutations identified
Advertisement
More than one-fifth of all human cancers harbor mutations in one of the members of the BAF chromatin remodeling complex. Deep biochemical and epigenomic characterization of a cell line panel comprehensively representing all these mutations enabled researchers at the CeMM Research Center for Molecule Medicine of the Austrian Academy of Sciences to identify new approaches to target BAF mutant cancers. The study describing these findings has now been published in the journal Nature Genetics.
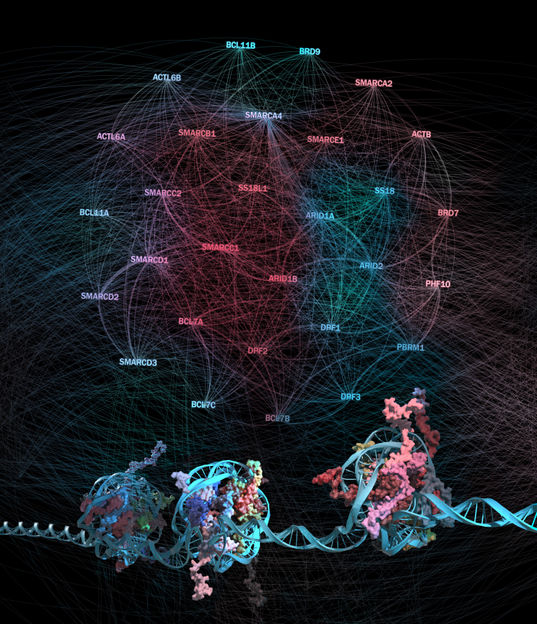
Protein-protein interaction network between subunits of the BAF chromatin remodeling complexes and their connection to chromatin regions they regulate
© CeMM/Bobby Rajesh Malhotra
Chromatin organizes the approximately two meters of DNA present in the nucleus of every human cell so that, dependent on the cell type and state, certain genes can be activated, others repressed. The fundamental organizing unit of chromatin is the nucleosome, consisting of 146 base pairs of DNA wrapped around a histone octamer. Whenever a cell needs to adapt – for example, to respond to developmental or environmental signals or to DNA damage –, it needs to alter the accessibility of its DNA. Doing exactly this is the function of chromatin remodelers, enzymes that use the energy of ATP to move or evict nucleosomes. Chromatin remodeling complexes come in multiple flavors in human cells; a particularly interesting complex is the BAF complex. In fact, it is not only one complex, but many different ones. Up to 15 complex positions can be occupied by proteins encoded from 29 different genes, the combinatorics adding up to more than 10,000 theoretically possible different complexes.
What makes the BAF complex so relevant for human disease are the mutations that are found in the BAF complex genes in approximately every fifth human cancer. Currently, we have only a limited understanding how these mutations contribute to cancer development. Even more problematic, we do not have therapies to specifically cure BAF mutant cancers. Finding such therapies is challenging, because typically the genetic aberrations are so called loss of function mutations. These result in cancer cells lacking a specific BAF subunit protein, and it is hard to develop a drug against something that is not there.
To find ways to nevertheless target BAF mutant cells, Sandra Schick, postdoctoral fellow in the laboratory of Stefan Kubicek of the CeMM Research Center for Molecular Medicine of the Austrian Academy of Sciences, first needed to generate a relevant cellular model. She therefore established a panel of 22 isogenic cell lines that differed only in each lacking a single different BAF subunit. In these cells, she first characterized the consequences of loss of a single subunit on complex composition, chromatin accessibility and transcription. “We identified preferential BAF complex configurations, which can be altered when single subunits are lost” said Schick. “Furthermore, there is an intense cross-talk between these subunits, so that, depending on the lost gene, other BAF subunits are incorporated with higher or lower frequency”. These data indicate that although the original mutation results in the loss of one BAF subunit, the cancer promoting properties might be conferred by aberrant functions of the remaining BAF complexes. And such aberrant functions might again be druggable.
To test whether it is indeed the case that BAF mutant cancers become addicted to the function of the remaining complexes, the team went on to systematically deplete a second member of the BAF complexes in these cells that had already lost one subunit. From this large dataset they focused on three novel intra-complex synthetic lethalities, SMARCA4-ARID2, SMARCA4-ACTB, and SMARCC1-SMARCC2. The extensive systematic data on interaction proteomics, chromatin accessibility and transcription changes helped explain the molecular mechanism for these synthetic interactions. “But even more important to us was to prove that these novel targets hold up in relevant cancer cell lines beyond our cellular model system” explains Stefan Kubicek. And this is exactly what the researchers could prove, in a panel of 22 different cancer cell lines. “The SMARCC1-SMARCC2 pair was particularly strong and conserved, and we could show that cell lines with low SMARCC1 levels are extremely sensitive to loss of SMARCC2.”
The project, conducted in the context of the Christian Doppler Laboratory for Chemical Epigenetics in collaboration with Boehringer Ingelheim, provided not only a deep molecular insight in the biochemical and epigenetic alterations after the loss of a BAF subunit, but also identified novel targets towards the goal of developing targeted treatments for BAF-mutated cancers.