Obesity risk quantification: a jump towards the future through the lens of artificial intelligence applied to lipid science
Scientists and biotech start-up Lipotype teamed up
Advertisement
According to WHO, nearly 1 out of 6 adults is obese. This makes obesity a prime threat to human health because it increases mortality and morbidity. In daily healthcare practice, the go-to indicator of overweight and obesity is the body mass index (BMI), a calculated relation between body weight and height. An international team of scientists led by Dresden researchers, with a joint effort between academy and industry in Saxony (Germany) introduces a revolutionary approach towards personalized and precision biomedicine. The discovery is that artificial intelligence can assist to design markers composed of a small combination of lipids that allow to provide significantly more information about obesity than BMI.

mohamed_hassan, pixabay.com, CC0
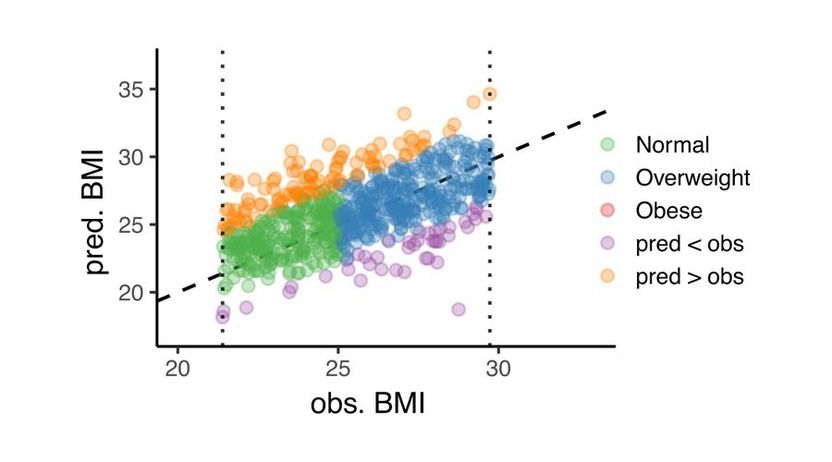
Comparison of observed BMI and predicted BMI.
© Gerl et al

When academy meets industry significant jumps towards the future are possible. Researchers from the Biotechnology Center (BIOTEC) at the TU Dresden and Lipotype GmbH, a spin-off of the Max Planck Institute for Molecular Cell Biology and Genetics, Dresden, with the international participation of scientists from Lund University (Sweden) and National Institute for Health and Welfare (Finland) teamed up to critically investigate the BMI of more than 1000 patients. The international research team applied advanced artificial intelligence tools to develop an algorithm which makes use of the human blood plasma lipid composition, the plasma lipidome.
The plasma lipidome contains hundreds of distinct lipids. “Together, they are valuable indicators to explore the state of metabolism health of an individual - like a health fingerprint”, explains Mathias Gerl from Lipotype. This lipidomic data was used for training the algorithm to predict the BMI of each patient.
In comparison to the ‘household measures’-based BMI (observed BMI), the lipidomic data provided the new algorithm with the power to propose a new ‘molecular lipidomic BMI’ (predicted BMI). The lipidomic BMI calculation revealed that the molecular BMI was in a number of cases significantly higher than the traditional BMI. In approximately 1 out of 7 patients, the lipidomic BMI improved the classic ‘morphometric BMI’, and provided more information about obesity compared to the traditional BMI measurement, e.g. about the amount of visceral fat, a harmful kind of fat deposit.
“Long-time consequences can occur when a patient in need for a weight reducing therapy to combat the risk for obesity-associated disease is sent home without remedy”, states Olle Melander from Lund University. “These patients may suddenly suffer from a heart attack at age 40 leaving their doctors puzzled”, comments Carlo Vittorio Cannistraci from BIOTEC at the TU Dresden and adds: “We should overcome the obsolete logic that a single marker can help to assess risk in complex systems such as humans. Computational biomedicine adopts artificial intelligence to design multidimensional markers composed of many variables that increase precision of diagnosis. Hence, we hope that the traditional BMI will be replaced with a lipidomic marker to outpace the misclassification of 14% of patients.”
Original publication
Mathias J Gerl, Christian Klose, Michal A Surma, Celine Fernandez, Olle Melander, Satu Männistö, Katja Borodulin, Aki S Havulinna, Veikko Salomaa, Elina Ikonen, Carlo V Cannistraci & Kai Simons; "Machine learning of human plasma lipidomes for obesity estimation in a large population cohort"; PLOS Biology; 2019
Other news from the department science
Most read news
More news from our other portals
Something is happening in the life science industry ...
This is what true pioneering spirit looks like: Plenty of innovative start-ups are bringing fresh ideas, lifeblood and entrepreneurial spirit to change tomorrow's world for the better. Immerse yourself in the world of these young companies and take the opportunity to get in touch with the founders.


























































