Seeing cancer’s spread through a computational window
Computational model allows researchers to simulate cellular-scale interactions across unprecedented distances in the human vasculature
Advertisement
Biomedical engineers at Duke University have significantly enhanced the capabilities of a computational model that simulates the movement of individual cancer cells across long distances within the entire human body.
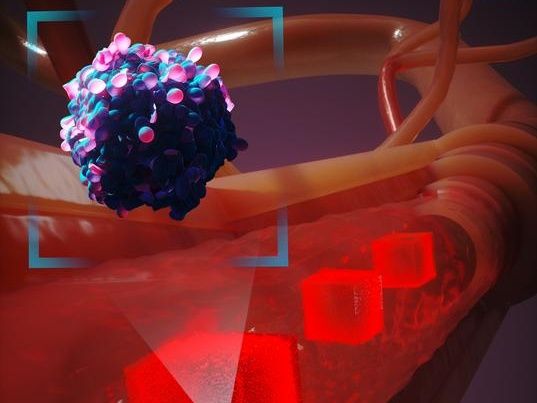
An artistic rendition of how a new computational modeling system simulates a cancer cell traveling through the human body. To account for millions of cellular interactions, it only creates detailed simulations of cells in the immediate vicinity of the cancer cell as it circulates in the blood stream.
Duke University
Called “Adaptive Physics Refinement (APR),” the approach captures detailed cellular interactions and their effects on cellular trajectory, offering invaluable insights into the travels of metastatic cancer cells.
“Cancer cells in our bloodstream are influenced by bumping off of and moving around nearby red blood cells and other cellular interactions,” said Aristotle Martin, a PhD candidate in the Amanda Randles laboratory at Duke Biomedical Engineering. “But it’s impossible to simulate the movement of every red blood cell in all of the body’s blood vessels, so we had to find a way to work around those computational limitations.”
The research was presented November 15, 2023, at the International Conference for High Performance Computing, Networking, Storage, and Analysis (SC23). This conference is the premier international meeting in the field of high-performance computing, sponsored by ACM and IEEE-CS.
Deciphering the dynamics of how cancer cells navigate through the body’s blood vessels remains a critical and complex issue in cancer studies, crucial for early detection and potential targeted treatment. Studying these processes in living patients, however, is not feasible, and instead requires advanced computational models to simulate cancer cell dynamics.
Amanda Randles, the Alfred Winborne and Victoria Stover Mordecai Associate Professor of Biomedical Sciences at Duke, has been creating and advancing computational methods that explore these fundamental processes for over a decade. One of her notable contributions is HARVEY, a highly scalable hemodynamics simulation package designed to operate on the world’s most advanced supercomputers.
But even supercomputers have their limits.
To calculate the trajectory of a single cancer cell, models must capture its microscopic interactions with the surrounding red blood cells. The human body, however, contains around 25 trillion red blood cells and five liters of blood. Using today’s largest supercomputers, state-of-the-art models can only recreate a region containing one percent of this volume at cellular resolution — a limited domain that still includes several hundred million red blood cells.
To skirt this issue, a large team with collaborators from Lawrence Livermore National Laboratory (LLNL) and Oak Ridge National Laboratory (ORNL) led by Sayan Roychowdhury, a former PhD student in the Randles laboratory, has taken a new approach. Extending the lab’s existing algorithm to include interactions with millions of neighboring red blood cells, APR creates a high-resolution window that tracks the cell of interest as it moves through the vasculature.
Part of the trick to making this approach work is coupling the moving window to a simulation of the entire vascular domain, modeling the blood as a bulk fluid. This approach is analogous to simulating a toy boat's behavior while floating down a stream. The simplest approach would be to model the entire waterway at the highest resolution from start to finish. However, in such a scenario, the vast majority of computational resources would precisely capture physical phenomena that occur far from the boat, which would be impractical at best.
Instead, it is far more efficient to model the region near the boat as accurately as possible while modeling the rest of the stream at more modest resolution. As the boat nears complex features such as rocks, eddies and rapids, the model would capture them precisely once they are close enough to have a measurable impact on the boat’s trajectory. The result is an accurate simulation that is far more efficient, allowing the simulation to explore much longer stretches of river.
"The most cells that we have ever simulated at one time is 580 million,” said Samreen Mahmud, a PhD student in the Randles Lab. “Our goal was to maximize the window size to see how many cells we could capture using a leadership class supercomputer. We then focused on reducing the computational cost and efficiently moving the method to the cloud.”
The efficiency of the algorithm in performing large-scale simulations was showcased in the study by simulating a cancer cell’s transit across a centimeter using only a single node on Amazon’s Web Services (AWS) for 500 hours. By employing Adaptive Physics Refinement, the computational memory demand was drastically decreased from petabytes to more manageable gigabytes.
The results, the researchers say, could be a game-changer for other laboratories studying cancer or developing biomedical devices. It could, for example, help researchers understand the mechanical and physical side of cancer metastasis by isolating factors that would be difficult or even impossible to do within an experimental setup. It also represents a significant leap in high-performance computing capabilities, facilitating the practical application of modeling vast quantities of red blood cells with constrained capacity.
Moving forward, the team plans to continue adding features to their modeling software, such as adhesion between cells and changes in cellular behavior near blood vessel walls. They also want to investigate how clusters of cancer cells move through the vasculature, as clinical studies have shown that traveling in groups increases metastatic cells’ potential to form new tumors.
“We are hoping that methods like APR will help democratize cellular-scale computational modeling by leveling the playing field,” Randles said, “We want to allow researchers without access to the world’s biggest supercomputers to use computational approaches to study cancer dynamics.”
Original publication
Sayan Roychowdhury, Samreen T. Mahmud, Aristotle Martin, Peter Balogh, Daniel F. Puleri, John Gounley, Erik W. Draeger, Amanda Randles; "Enhancing Adaptive Physics Refinement Simulations Through the Addition of Realistic Red Blood Cell Counts"; Proceedings of the International Conference for High Performance Computing, Networking, Storage and Analysis, 2023-11-11