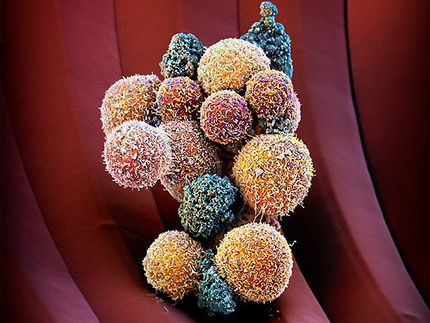
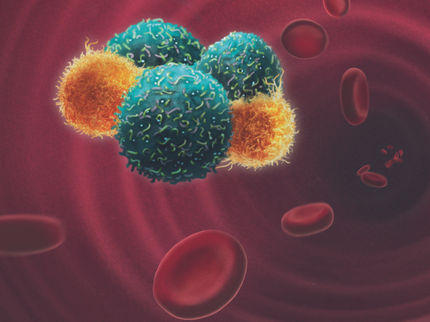
A lack of oxygen in tumors promotes metastasis
Important starting point for the development of new cancer treatments
Advertisement
metastases are formed by cancer cells that break away from the primary tumor. A research group at the University of Basel has now identified lack of oxygen as the trigger for this process. The results reveal an important relationship between the oxygen supply to tumors and the formation of metastases. This research may open up new treatment strategies for cancer.
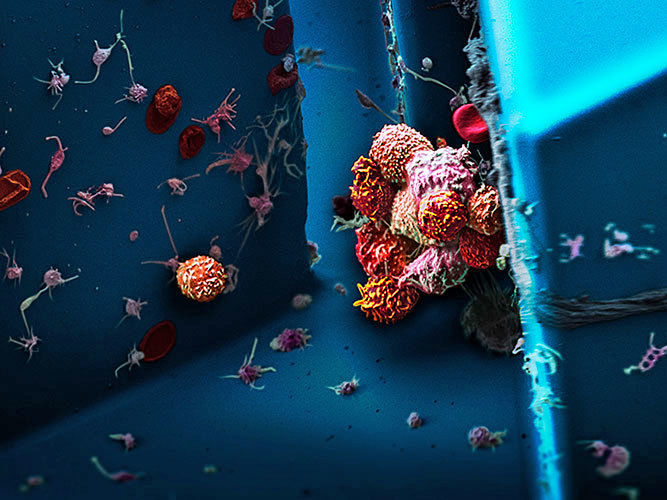
Clusters of circulating tumor cells, isolated from the blood of a patient with breast cancer, examined under a scanning electron microscope.
Martin Oeggerli/Micronaut, supported by Nicola Aceto & Ali Fatih Sarioglu
The chances of recovery significantly worsen when a tumor metastasizes. Previous research has shown that metastases are formed by clusters of cancer cells that separate from the primary tumor and migrate to new tissue through the bloodstream. However, thus far little has been known about why these clusters of circulating tumor cells (CTCs) leave the tumor in the first place.
Lack of oxygen leads to more metastases
Professor Nicola Aceto’s research group at the University of Basel’s Department of Biomedicine has now shown that a lack of oxygen is responsible for the separation of CTC clusters from the tumor. This is an important starting point for the development of new cancer treatments.
A mouse model for breast cancer formed the basis of the experiments: the researchers analyzed the oxygen supply inside these tumors, which are equivalent to human cancer tissue, the detachment of CTCs and their molecular and cell biological properties.
It turned out that different areas of a tumor are supplied with different levels of oxygen: cancer cells with a lack of oxygen were found wherever the tumor had comparatively fewer blood vessels – in the core of the tumor as well as in clearly defined peripheral areas. Next, the research team investigated the CTC clusters that had separated from these tumors and found that they similarly suffered from a lack of oxygen. This led to the conclusion that cells leave the tumor if they do not receive enough oxygen. “It’s as though too many people are crowded together in a small space. A few will go outside to find some fresh air,” says Aceto.
Further experiments showed that these CTC clusters with a lack of oxygen are particularly dangerous: in comparison to clusters with normal oxygen content, they formed metastases faster and shortened the mice’s survival time. “If a tumor does not have enough oxygen, these CTC clusters, which have a particularly high potential to develop metastases, will break away,” says Aceto.
Stimulating blood vessel formation as a treatment approach
This insight led the researchers to take a closer look at the effect of what is called proangiogenic treatment: they stimulated the formation of blood vessels, thus boosting the supply of oxygen to the tumor cells. As expected, the number of separating CTC clusters dropped, the mice formed fewer metastases, and they lived longer – but at the same time, the primary tumor increased in size significantly.
“This is a provocative result,” says Aceto. “If we give the tumor enough oxygen, the cancer cells have no reason to leave the tumor and metastasize. On the other hand, this accelerates the growth of the primary tumor.”
The next challenge is to transfer these findings to a clinical environment, where the characteristics of tumors vary from patient to patient: “But we speculate that substances that improve oxygen supply to the tumor can inhibit the formation of metastases in breast cancer, alone or in combination with other agents.”
Original publication
Cinzia Donato, Leo Kunz, Francesc Castro-Giner, Aino Paasinen-Sohns, Karin Strittmatter, Barbara Maria Szczerba, Ramona Scherrer, Nunzia Di Maggio, Wolf Heusermann, Oliver Biehlmaier, Christian Beisel, Marcus Vetter, Christoph Rochlitz, Walter Paul Weber, Andrea Banfi, Timm Schroeder & Nicola Aceto; "Hypoxia Triggers the Intravasation of Clustered Circulating Tumor Cells"; Cell Reports; 2020